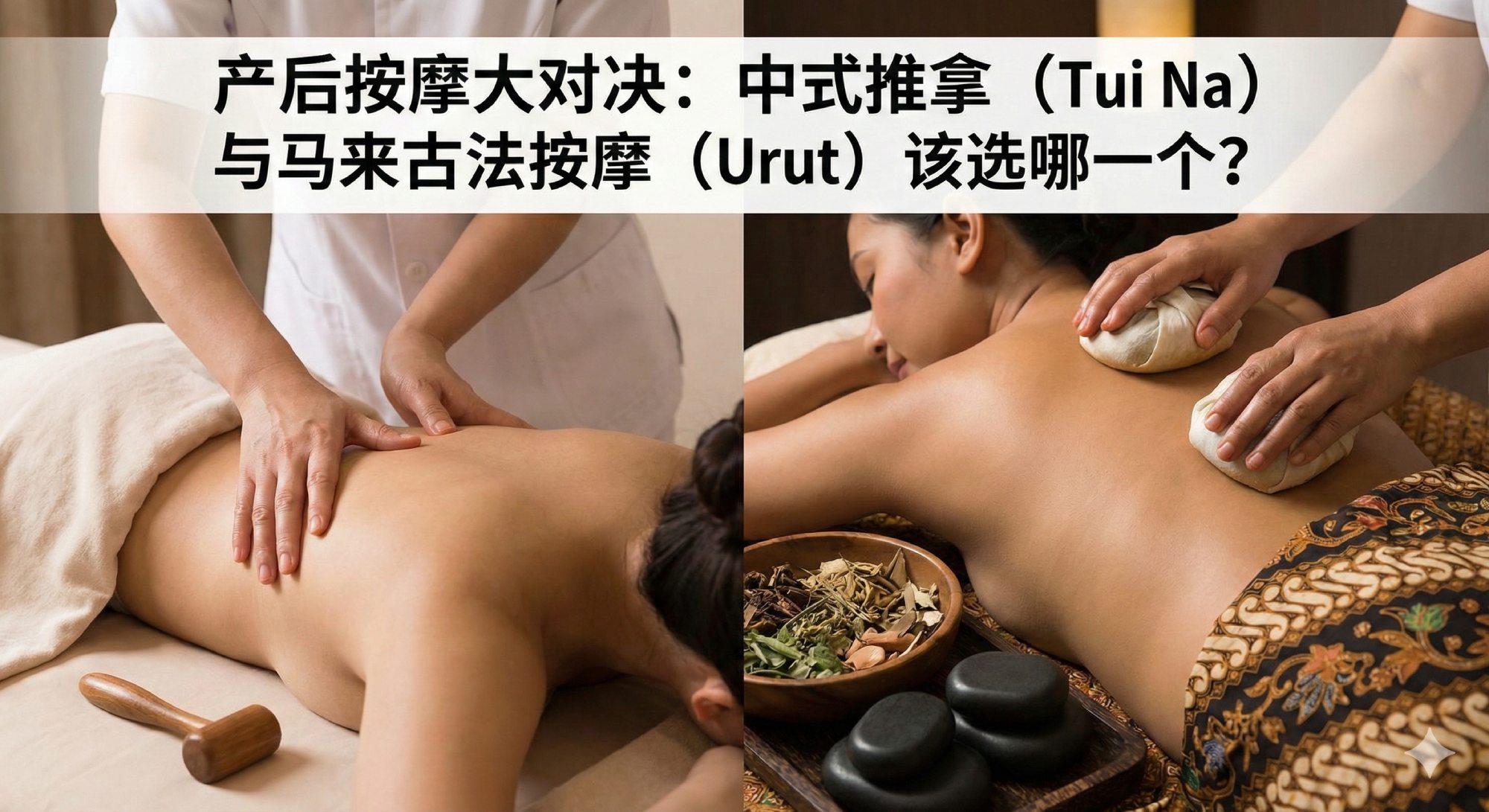
Chinese vs Malay Postnatal Massage: Tui Na vs Urut (2026 Malaysian Mom Guide)
Staring at the menu of postnatal massage services, wondering whether to book Tui Na or Urut? You are not alone. For Malaysian new moms, this decision feels overwhelming—especially when every auntie has a different opinion.
Here is the truth: both Chinese and Malay postnatal massage traditions have healed generations of mothers. But they work differently. Choosing the right one (or combining both) depends on your body, your delivery, and your recovery goals.
In this guide, we break down everything—techniques, benefits, rituals, and price ranges—so you can make the best choice for your postnatal massage in Malaysia.
Quick Comparison: Tui Na vs Urut at a Glance
| Feature | Chinese Tui Na (推拿) | Malay Urut Pantang |
|---|---|---|
| Main Focus | Pain relief, expelling “wind,” muscle recovery | Lactation support, womb repositioning, body shaping |
| Technique | Deep acupressure on meridian points | Long, rhythmic strokes with herbal oils |
| Pressure Level | Firm to intense (deep tissue) | Moderate to firm (relaxing) |
| Special Rituals | Ginger oil application, meridian stimulation | Sengkak (womb lifting), Bertungku (hot stone), Bengkung binding |
| Best For | Back pain, joint stiffness, C-section recovery | Breastfeeding moms, womb recovery, waist slimming |
| Typical Price (KL/PJ) | RM150–300 per session | RM180–350 per session |
Traditional Malay Massage (Urut Pantang): The Holistic Healer
Urut Pantang is more than a massage—it is a full postpartum wellness system passed down through Malay midwives (bidan) for centuries.
The Technique: Rhythmic & Relaxing
Using thumbs, palms, and forearms, the therapist applies long, flowing strokes with warmed herbal oils (often lemongrass or ginger-infused). The pressure is firm but soothing—designed to:
- Improve blood circulation
- Stimulate lymphatic drainage
- Release “angin” (wind) from the body
- Relax tense muscles from labor
The Lactation Advantage: Urut Payudara
Here is where Malay massage truly shines for breastfeeding moms. Therapists perform Urut Payudara—specialized breast and underarm massage that:
- Clears blocked milk ducts
- Relieves engorgement pain
- Stimulates milk production
- Drains lymph nodes to prevent mastitis
If you are struggling with low milk supply or frequent clogged ducts, this alone makes Urut worth considering.
Unique Rituals: Sengkak & Bertungku
Sengkak (Womb Lifting): A gentle but specific technique where the therapist uses controlled pressure to guide the uterus back to its pre-pregnancy position. This helps with:
- Faster uterine involution
- Reduced postpartum bleeding
- Better pelvic floor recovery
Bertungku (Hot Stone Therapy): A heated river stone wrapped in medicinal leaves is pressed along the abdomen and back. Benefits include:
- Breaking down residual fat deposits
- Expelling “cold wind” from the body
- Improving circulation to healing tissues
Bengkung Binding: Post-massage, your abdomen is wrapped tightly with a long cotton cloth. This traditional corset:
- Supports the pelvic floor
- Helps diastasis recti recovery
- Reshapes the waistline naturally
Traditional Chinese Massage (Tui Na): The Precision Fixer
Tui Na (pronounced “twee nah”) comes from Traditional Chinese Medicine (TCM) principles. It views postpartum recovery as restoring balance to the body’s energy flow (Qi) and blood circulation.
The Technique: Targeted & Therapeutic
Unlike the flowing strokes of Urut, Tui Na uses:
- Thumb and finger pressure on specific acupoints
- Elbow techniques for deeper muscle release
- Meridian line stimulation to unblock energy pathways
The pressure is typically more intense—digging into knots and tension points rather than gliding over them.
Focus: Pain Relief & “Wind” Expulsion
TCM theory says childbirth leaves the body vulnerable to “Wind-Dampness”—a condition causing:
- Chronic back pain
- Stiff joints and muscle tension
- Sensitivity to cold and drafts
- Persistent body aches
Tui Na directly addresses these issues by:
- Stimulating blood flow to injured tissues
- Releasing deep muscle tension
- Warming the body from within using ginger oil
- Restoring proper alignment
If you left the hospital with severe back pain or feel like your body “never recovered” from labor, Tui Na may provide the deep tissue relief you need.
Post-C-Section Considerations
Many Chinese massage therapists have specific protocols for Caesarean recovery, focusing on:
- Scar tissue mobilization (after healing)
- Abdominal muscle reconnection
- Improving digestion and bloating
Which Postnatal Massage Should YOU Choose?
Still torn? Here is a simple decision framework based on your biggest postpartum concerns:
Choose Malay Urut If:
- ✅ You are breastfeeding and need lactation support
- ✅ You want womb repositioning (Sengkak)
- ✅ Waist slimming/body shaping is a priority
- ✅ You prefer a relaxing, oil-based massage
- ✅ You love traditional hot stone (Bertungku) therapy
Choose Chinese Tui Na If:
- ✅ You have severe back/joint pain from pregnancy
- ✅ You feel “cold” or have wind sensitivity
- ✅ You want deep tissue work for muscle knots
- ✅ You had a C-section and need scar recovery
- ✅ You prefer acupressure over oil massage
Can You Combine Both? The Fusion Approach
Yes—and many Malaysian moms do!
Modern confinement centers and mobile massage services now offer fusion packages that blend the best of both traditions:
- Start with Tui Na to fix back pain and muscle tension
- Follow with Urut for breast care and womb lifting
- End with Bengkung binding for support
Talk to your therapist about your specific needs. Many are cross-trained in both techniques and can customize your session.
Frequently Asked Questions (FAQ)
When can I start postnatal massage?
For natural birth: As early as 3–5 days postpartum, once bleeding stabilizes.
For C-section: Wait 4–6 weeks until the incision is fully healed. Always get clearance from your doctor first.
How many sessions do I need?
Traditional confinement massage packages typically include 7–10 sessions over 2–4 weeks. For specific issues like back pain or low milk supply, 3–5 targeted sessions may suffice.
Is postnatal massage painful?
Malay Urut is generally relaxing with moderate pressure. Chinese Tui Na can be intense—especially on sore spots—but should not be unbearable. Always communicate with your therapist about pressure preferences.
Can I do postnatal massage if I am not breastfeeding?
Absolutely! Both Tui Na and Urut offer benefits beyond lactation—womb recovery, pain relief, and emotional wellness apply to all new mothers.
How much does postnatal massage cost in Malaysia?
Prices vary by location and experience:
- Mobile/home service: RM180–350 per session
- Confinement centers: Often included in packages
- 7-session package: RM1,200–2,500
What should I avoid after postnatal massage?
- ❌ Cold drinks or showering immediately after
- ❌ Heavy lifting or strenuous exercise
- ❌ Sexual intercourse for at least 2 weeks
- ✅ Do drink warm water and rest
Final Thoughts: Listen to Your Body
There is no “wrong” choice between Tui Na and Urut. Both traditions have stood the test of time because they work.
The best postnatal massage is the one that addresses your recovery needs—whether that is fixing your aching back, boosting your milk supply, or simply giving yourself permission to rest and heal.
Our advice? If you can, try both. Start with one tradition for a few sessions, then switch. Notice how your body responds. The goal is not perfection—it is recovery, one massage at a time.
Have you tried Tui Na or Urut? Which worked better for your recovery? Share your experience in the comments below—we would love to hear from you!

Private Part Smell: How Your Diet Affects Taste and Odor Down There
When it comes to intimacy and personal hygiene, we often focus on soaps, washes, and grooming habits. However, one of the most significant factors influencing your body’s natural scent and taste comes from within. The age-old adage “you are what you eat” applies surprisingly well to your bodily fluids. Your diet plays a pivotal role in regulating your body’s pH balance, which directly impacts private part smell and taste.
The Connection Between Diet and Body Chemistry
Your body is a complex chemical laboratory. Everything you ingest is broken down and processed, and the byproducts of this metabolism are excreted through sweat, urine, and other bodily fluids. Because mucous membranes are highly permeable, the foods that are potent enough to change the smell of your breath or urine are often potent enough to alter the scent and taste of your reproductive fluids.
While every individual has a unique natural scent, certain food groups can intensify odors or sweeten the taste. Understanding which foods do what can help you feel more confident and fresh during intimate moments.
Foods That May Negatively Impact Smell and Taste
If you are noticing a stronger or more pungent odor than usual, your last few meals might be the culprit. Here are some common foods that are known to negatively affect bodily scents.
Red Meat
While a steak dinner might sound romantic, it may not be the best choice right before intimacy. Red meat is chemically complex and can be difficult for the body to digest. It often leaves behind a residue that can make bodily fluids taste salty and smell stronger. The high protein content and specific enzymes required to break down red meat can result in a heavier, muskier scent released through the pores and fluids.
Dairy Products
Dairy is another culprit that can throw off your natural balance. For many people, dairy products like cheese, milk, and cream can increase mucus production. In terms of taste and smell, excessive dairy consumption has been colloquially associated with a “curdled” or more acidic profile in bodily fluids. If you are sensitive to lactose, the digestive upset can further contribute to unpleasant body odors.
Strong Spices, Garlic, and Onions
It is well known that garlic and onions cause bad breath, but their sulfur-containing compounds don’t stop there. These compounds are absorbed into the bloodstream and expelled through the lungs and pores. Consequently, they can impart a strong, distinct odor to vaginal fluids and semen. Similarly, strong spices like curry can linger in the body’s secretions for hours or even days after consumption.
Asparagus
Asparagus is famous for causing a distinct, pungent odor in urine shortly after eating it. This is due to the breakdown of asparagusic acid. While the effect is most noticeable in urine, the chemical compounds can also slightly alter the pH and scent of other fluids in the pelvic region.
Caffeine and Alcohol
Both coffee and alcohol are diuretics, meaning they dehydrate the body. Dehydration concentrates bodily fluids, making any natural taste or smell much more potent and often bitter. Alcohol, in particular, can create an acidic environment in the body, which is not ideal for maintaining a fresh scent.
Foods That Improve Taste and Smell
Just as some foods can make things worse, others act as natural deodorizers and sweeteners. Incorporating these into your diet can lead to a milder, sweeter, and more pleasant experience.
Pineapple and Citrus Fruits
Pineapple is perhaps the most famous food recommended for improving the taste of private parts. It is rich in natural sugars and enzymes that can sweeten bodily fluids. Similarly, citrus fruits like oranges, lemons, and grapefruits are high in Vitamin C and antioxidants. These help the body flush out toxins and maintain a healthy, balanced pH level, leading to a fresher scent.
Cranberries
Cranberry juice is widely recognized for supporting urinary tract health, but it also helps balance pH levels in the body. By fighting off harmful bacteria and increasing acidity in the urine (which prevents bacterial growth), cranberries can help maintain a clean and neutral scent.
Water and High-Water Content Vegetables
The ultimate solution to pollution is dilution. Drinking plenty of water is the single most effective way to improve private part smell. Hydration dilutes the compounds in your sweat and fluids, making them milder. Vegetables with high water content, such as celery and parsley, also help. Parsley, in particular, contains chlorophyll, which acts as a natural internal deodorizer.
Cinnamon and Peppermint
Spices aren’t all bad. Sweet spices like cinnamon and fresh herbs like peppermint can improve the flavor profile of bodily fluids. Unlike heavy savory spices, these tend to leave a milder, sweeter, or fresher trace.
Conclusion
While hygiene is essential, your diet is a powerful tool in managing private part smell. You don’t need to completely eliminate foods you love, but being mindful of your intake before intimacy can make a difference. Moderating red meat, dairy, and alcohol while increasing your intake of water, fruits, and vegetables can boost your confidence and improve your body’s natural chemistry.
Understanding Uterine Prolapse: Symptoms, Causes, and Effective Treatments
Uterine prolapse is a medical condition that affects many women, yet it remains a topic often shrouded in silence due to embarrassment or lack of awareness. Simply put, uterine prolapse (known as 子宫下垂 in Chinese medical contexts) occurs when the pelvic floor muscles and ligaments stretch and weaken, providing inadequate support for the uterus. Consequently, the uterus slips down into or protrudes out of the vagina.
While this condition can affect women of any age, it is most common in postmenopausal women who have had one or more vaginal deliveries. Understanding the signs, causes, and treatment options is crucial for maintaining long-term pelvic health and quality of life.
What Exactly is Uterine Prolapse?
The uterus (womb) is normally held in place inside the pelvis with various muscles, tissue, and ligaments. Think of these support structures as a hammock. When this hammock weakens or gets damaged, it can no longer hold the uterus in its proper position. Gravity takes over, and the uterus descends toward the vaginal opening.
Prolapse can range from mild to severe:
- First degree: The cervix drops into the vagina.
- Second degree: The cervix drops to the level just inside the opening of the vagina.
- Third degree: The cervix is outside the vagina.
- Fourth degree: The entire uterus is outside the vagina (procidentia).
Identifying the Symptoms
In mild cases, women may not experience any noticeable symptoms. However, as the condition progresses, the signs become more apparent and can significantly impact daily life. Common symptoms include:
- A sensation of heaviness or pulling in the pelvis.
- Tissue protruding from the vagina, often described as feeling like you are sitting on a small ball.
- Urinary problems, such as urine leakage (incontinence) or urine retention (inability to empty the bladder completely).
- Trouble having a bowel movement.
- Lower back pain that often worsens as the day goes on.
- Sexual concerns, such as a sensation of looseness in the tone of your vaginal tissue.
Symptoms are often less bothersome in the morning and worsen as the day progresses due to the effects of gravity.
Causes and Risk Factors
Several factors contribute to the weakening of the pelvic floor muscles, leading to uterine prolapse. It is rarely caused by a single event but rather a combination of factors over time.
1. Pregnancy and Childbirth
This is the most significant risk factor. Pregnancy puts immense strain on the pelvic floor, and vaginal childbirth—especially with a large baby or difficult labor—can stretch and tear the supportive tissues. The damage may not manifest as prolapse until years later.
2. Aging and Menopause
As women age, the natural production of estrogen decreases. Estrogen helps keep the pelvic muscles strong and elastic. During menopause, the drop in estrogen levels leads to thinner, less resilient pelvic tissues, increasing the risk of prolapse.
3. Chronic Strain
Any activity that puts repeated pressure on the abdomen can weaken pelvic muscles. This includes:
- Chronic coughing (often associated with smoking or lung conditions).
- Straining during bowel movements (chronic constipation).
- Heavy lifting, whether for exercise, work, or daily chores.
4. Obesity
Excess body weight places additional strain on the pelvic floor muscles, accelerating their weakening.
Diagnosis and Treatment Options
If you suspect you have uterine prolapse, consulting a healthcare provider is essential. Diagnosis is usually confirmed through a pelvic examination. Treatment depends on the severity of the prolapse and how much the symptoms affect your life.
Non-Surgical Treatments
For mild to moderate cases, or for women who wish to avoid surgery, conservative treatments are often effective:
- Lifestyle Changes: Losing weight, treating constipation, and avoiding heavy lifting can reduce pressure on the pelvic floor.
- Kegel Exercises: These exercises strengthen the pelvic floor muscles. When performed correctly and consistently, they can halt the progression of prolapse and alleviate symptoms.
- Vaginal Pessary: A plastic or rubber ring inserted into the vagina to support the bulging tissues. This is a common non-surgical solution that requires regular cleaning.
Surgical Interventions
For severe cases where conservative measures fail, surgery may be recommended. Options generally include:
- Tissue Repair: Grafting your own tissue, donor tissue, or synthetic material onto the weakened pelvic floor structures to support the pelvic organs.
- Hysterectomy: The removal of the uterus. This is often considered when the prolapse is severe and the woman does not plan to have more children.
Prevention and Outlook
While you cannot control genetic factors or aging, you can take steps to protect your pelvic floor. Maintaining a healthy weight, treating chronic coughs promptly, avoiding constipation through a high-fiber diet, and regularly performing pelvic floor exercises are the best defenses against uterine prolapse.
Uterine prolapse is a treatable condition. With the right medical guidance and lifestyle adjustments, women can regain their comfort and confidence. If you are experiencing symptoms, do not suffer in silence—reach out to a gynecologist to discuss the best path forward for your health.

Essential Guide to Recovery and Confinement After a Miscarriage
Experiencing a miscarriage is one of the most challenging events a woman can go through. It is a profound loss that affects not only the emotional state but also takes a significant physical toll on the body. While society often focuses on the emotional grief associated with pregnancy loss, the physical recovery process is equally critical. Just as with a full-term delivery, the body requires a dedicated period of rest, often referred to in various cultures as “confinement,” to heal properly.
Understanding the Physical Toll of Miscarriage
Regardless of when the miscarriage occurs during the pregnancy, the body undergoes substantial hormonal and physiological changes. Following the loss, the uterus must contract back to its pre-pregnancy size, a process that can involve cramping and bleeding similar to a heavy period. This is the body’s natural way of healing, but it requires energy and resources.
During this time, your hormone levels—specifically estrogen and progesterone—drop rapidly. This chemical shift can exacerbate feelings of sadness and fatigue. Understanding that these physical symptoms are a normal part of the recovery process can help you be kinder to yourself during this difficult time.
The Importance of a “Confinement” Period
In many Asian cultures, the concept of “berpantang” or confinement is strictly observed after childbirth. However, health experts increasingly advocate for a modified version of this rest period following a miscarriage as well. Treating the post-miscarriage period with the same seriousness as postpartum recovery is essential for long-term health.
Rest and Activity Restrictions
The primary goal of confinement after a miscarriage is to allow the reproductive organs to heal. Medical professionals generally recommend the following:
- Avoid Heavy Lifting: Straining the abdominal muscles can interfere with the healing of the uterus. Avoid lifting heavy objects, including other children, for at least two weeks.
- Prioritize Sleep: Your body repairs itself while you sleep. Fatigue is common as your blood volume readjusts, so listen to your body and nap when needed.
- Pelvic Rest: To prevent infection, doctors typically advise avoiding sexual intercourse, tampons, and douching until the bleeding has completely stopped and the cervix has closed. This usually takes about two weeks, but you should consult your healthcare provider for a specific timeline.
Nutritional Support for Healing
Diet plays a pivotal role in how quickly you recover physically. During the confinement period, your body needs to replenish lost nutrients, particularly iron and vitamins.
- Iron-Rich Foods: Blood loss during a miscarriage can lead to anemia or low energy. Incorporate red meat, spinach, beans, and lentils into your diet to boost iron levels.
- Vitamin C: To help your body absorb iron effectively, pair iron-rich foods with sources of Vitamin C, such as oranges, strawberries, and bell peppers.
- Hydration: Drinking plenty of water is crucial for hormonal balance and general recovery. Warm fluids, such as soups and herbal teas, are often recommended in traditional confinement practices to maintain body warmth and improve circulation.
- Avoid “Cold” Foods: Drawing from traditional wellness advice, many women find comfort in avoiding foods considered “cooling” to the body, such as iced drinks or certain raw vegetables, to prevent bloating and discomfort during the healing phase.
Navigating Emotional Grief
Healing is not just physical; it is deeply emotional. The sudden end of a pregnancy can bring about a complex mix of shock, guilt, anger, and profound sadness. It is important to acknowledge that grief has no set timeline.
Communication with your partner is vital. They are also grieving, though perhaps in a different way. creating a space where both of you can express your feelings without judgment can strengthen your bond. Additionally, seeking support from counselors or support groups specializing in pregnancy loss can provide a safe environment to process these emotions.
When to Seek Medical Attention
While some pain and bleeding are normal, it is crucial to monitor your recovery for signs of complications. You should contact your doctor immediately if you experience:
- Heavy Bleeding: Soaking through more than two maxi pads in an hour for two consecutive hours.
- Signs of Infection: Fevers, chills, or foul-smelling vaginal discharge.
- Severe Pain: Abdominal pain that is not relieved by prescribed pain medication or standard over-the-counter pain relievers.
Recovery takes time. Whether you call it confinement or simply a recovery period, giving yourself permission to rest is the single most important step you can take. By nourishing your body and honoring your emotions, you pave the way for healing and future well-being.

Understanding Vaginal Discharge: A Complete Guide to Intimate Health
Vaginal discharge, medically known as leukorrhea, is a topic that many women feel hesitant to discuss, yet it is a fundamental aspect of gynecological health. Understanding the nuances of your intimate area is crucial for overall well-being. While the presence of discharge is a normal physiological function, changes in its color, consistency, or odor can be the body’s way of signaling an underlying issue. This comprehensive guide will help you distinguish between normal bodily functions and potential infections, empowering you to take better care of your intimate health.
What is Leukorrhea?
Leukorrhea refers to the flow of a whitish, yellowish, or greenish discharge from the vagina of the female that may be normal or that may be a sign of infection. In its healthy state, vaginal discharge serves a vital housekeeping function. It is produced by glands inside the vagina and cervix to carry away dead cells and bacteria. This process keeps the vagina clean and helps prevent infection.
Normal discharge typically varies throughout your menstrual cycle. You might notice it is thinner and watery just after your period, becoming thicker and sticky (like egg whites) during ovulation. Recognizing your body’s baseline is the first step in identifying when something is wrong.
Distinguishing Normal from Abnormal Discharge
To maintain optimal intimate health, it is essential to know what to look for. Normal discharge is usually clear or milky white and does not have a strong, unpleasant smell. However, if the balance of healthy bacteria in your vagina is upset, the texture, color, and smell of your discharge may change.
Color Decoding: What Your Discharge Mean
- Clear and Watery: This is generally normal and healthy. It can occur at any time of the month and may be particularly heavy after exercise.
- White and Clumpy: If the discharge is thick, white, and resembles cottage cheese, it is a classic sign of a yeast infection. This is often accompanied by intense itching and irritation.
- Yellow or Green: Discharge that is a darker shade of yellow or green, especially if it is thick or accompanied by a bad smell, may indicate an infection such as trichomoniasis, which is often spread through sexual contact.
- Grayish: A gray hue combined with a strong, fishy odor is highly indicative of Bacterial Vaginosis (BV), the most common vaginal infection in women ages 15-44.
- Brown or Bloody: Brown discharge is usually just old blood leaving the body, often appearing right after your period ends. However, spotting between periods or bloody discharge could signal hormonal imbalances or other medical concerns that require a doctor’s visit.
Common Causes of Abnormal Discharge
Several factors can disrupt the delicate pH balance of the intimate area, leading to abnormal leukorrhea. Understanding these causes can help in prevention and early treatment.
Bacterial Vaginosis (BV)
BV occurs when there is an overgrowth of certain bacteria in the vagina. While the exact cause isn’t always clear, activities that change the bacterial balance, such as douching or having a new sex partner, can increase the risk. Symptoms often include the characteristic fishy odor and gray discharge mentioned earlier.
Yeast Infections (Candidiasis)
A yeast infection is caused by an overgrowth of a fungus called Candida. This fungus naturally lives in the vagina in small numbers, but stress, antibiotics, pregnancy, or uncontrolled diabetes can cause it to multiply rapidly, leading to the thick, white discharge and discomfort.
Trichomoniasis
This is caused by a parasite and is typically transmitted sexually. In addition to yellow-green discharge, it can cause pain during urination and itching. Unlike yeast infections, this requires prescription medication to treat effectively.
Best Practices for Intimate Hygiene
Maintaining a healthy intimate area isn’t just about treating infections; it is about prevention. Here are key lifestyle adjustments to support vaginal health:
- Avoid Douching: Douching can upset the natural balance of bacteria in the vagina and actually increase the risk of infection. The vagina is self-cleaning; warm water is usually sufficient for external cleaning.
- Choose Breathable Fabrics: Wear cotton underwear and loose-fitting clothing to keep the area cool and dry. Synthetic fabrics and tight pants can trap moisture, creating a breeding ground for bacteria and yeast.
- Practice Safe Sex: Using condoms can prevent sexually transmitted infections that cause abnormal discharge.
- Wipe Correctly: Always wipe from front to back after using the toilet to prevent bacteria from the anal region from entering the vagina.
- Manage Antibiotic Use: If you must take antibiotics for another condition, consider eating yogurt with live and active cultures or taking probiotics to help maintain healthy bacterial levels.
When to See a Doctor
While minor changes in discharge can occur due to hormonal shifts, certain symptoms warrant professional medical advice. You should consult a healthcare provider if:
- Your discharge changes color to green, yellow, or gray.
- You experience itching, burning, or swelling of the vagina or vulva.
- The discharge has a strong or foul odor.
- You have pelvic pain or pain during urination.
- You notice blisters or sores in the intimate area.
Your intimate health is a window into your overall well-being. By paying attention to the signs your body gives you through vaginal discharge, you can address issues early and maintain a healthy, comfortable lifestyle. If you are ever in doubt, it is always better to consult with a gynecologist rather than attempting to self-diagnose.

10 Common Reasons for an Itchy Vagina (And How to Stop the Itch)
There are few things more uncomfortable—or inconvenient—than an itchy vagina. It is the kind of nagging sensation that can distract you during a meeting, ruin a date, or keep you awake at night. While the immediate urge is to scratch, most women hesitate, knowing that scratching delicate tissue usually makes matters worse. Furthermore, the panic often sets in: Is it an infection? Is it something serious?
The first assumption many women make is that they have a yeast infection. While yeast is a very common culprit, it is far from the only reason you might be experiencing irritation “down there.” In fact, treating yourself for a yeast infection when you actually have a bacterial issue or a skin condition can delay proper healing and potentially exacerbate the problem.
Understanding the root cause of the itch is the first step toward relief. Below, we explore ten common reasons why your vagina (or more accurately, your vulva) might be itching, based on expert medical insights, and what you can do to stop the irritation.
1. Bacterial Vaginosis (BV)
Bacterial Vaginosis is actually the most common vaginal infection in women between the ages of 15 and 44. It occurs when the delicate balance of bacteria in the vagina is disrupted, allowing “bad” bacteria to outnumber the “good” lactobacilli. While itching is a symptom, the hallmark sign of BV is usually a thin, greyish-white discharge accompanied by a distinct, fishy odor.
How to handle it: Unlike a yeast infection, BV cannot be treated with over-the-counter creams. You will need to see a doctor for a prescription antibiotic, either in pill or gel form. Ignoring BV can increase your risk of contracting STIs, so medical attention is necessary.
2. Yeast Infections
While not the only cause, yeast infections are undeniably a major player in vaginal itching. These occur when there is an overgrowth of the fungus Candida. The itching associated with a yeast infection is often intense and internal as well as external. You may also notice a thick, white, clumpy discharge that resembles cottage cheese.
How to handle it: If you have had one before and recognize the symptoms, over-the-counter antifungal creams or suppositories are often effective. However, if this is your first time or the OTC medication doesn’t work, visit your gynecologist to rule out other strains of yeast or different infections.
3. Contact Dermatitis
Your vulva is covered in skin, and just like the skin on your face or arms, it can have an allergic reaction to irritants. This is known as contact dermatitis. If you have recently changed laundry detergents, started using a new body wash, or switched brands of toilet paper (especially scented ones), your skin might be protesting.
How to handle it: The solution here is elimination. Stop using scented soaps, bubble baths, and feminine hygiene sprays. Switch to hypoallergenic laundry detergent and avoid fabric softeners on your underwear. If the itch persists, a doctor might recommend a low-potency hydrocortisone cream to calm the inflammation.
4. Eczema or Psoriasis
If you suffer from skin conditions like eczema or psoriasis on other parts of your body, you can unfortunately develop them on your vulva as well. Eczema can manifest as red, itchy, and inflamed skin, while psoriasis often presents as thick, scaly red patches.
How to handle it: Because the skin in the genital area is thinner and more sensitive than elsewhere, you should not use the same strong prescription creams you might use on your elbows or knees. Consult a dermatologist or gynecologist for a treatment plan tailored to sensitive areas, which may include mild steroids or sitz baths.
5. Sexually Transmitted Infections (STIs)
Several STIs lists itching as a primary symptom. While the thought is frightening, identifying the issue is crucial for your health.
- Trichomoniasis: Caused by a parasite, this very common STI often causes itching, burning, and a frothy, yellow-green discharge with a foul smell.
- Herpes: Genital herpes often begins with tingling or itching before the appearance of painful blisters or sores.
- Pubic Lice (Crabs): Though less common today due to grooming habits, these parasites cause intense itching in the pubic hair region.
How to handle it: If you suspect an STI, get tested immediately. Treatments vary from antibiotics for Trichomoniasis to antiviral medications for Herpes management.

6. Hormonal Changes
Your hormones play a significant role in vaginal health. When estrogen levels drop—typically during menopause, perimenopause, or while breastfeeding—the vaginal wall can become thinner and drier. This condition, known as vaginal atrophy, often leads to itching and discomfort, particularly during sex.
How to handle it: Over-the-counter vaginal moisturizers and water-based lubricants can help with dryness. For more persistent cases, a doctor may prescribe a topical estrogen cream or a vaginal ring to restore moisture and elasticity.
7. Lichen Sclerosus
This is a chronic skin condition that is less common but serious. It causes patchy, white skin on the vulva that appears thinner than normal. It is most often seen in postmenopausal women but can affect anyone. The itching can be severe and may lead to scarring if left untreated.
How to handle it: Lichen Sclerosus requires a diagnosis from a medical professional, often confirmed by a biopsy. Treatment usually involves high-potency prescription steroid creams to reduce inflammation and prevent scarring.
8. Shaving and Grooming Habits
If you shave your bikini line, you are likely familiar with the itch that comes a day or two later as the hair grows back. Razor burn and folliculitis (infected hair follicles) are major sources of vulvar itching. The friction from tight clothing against freshly shaved skin can exacerbate the irritation.
How to handle it: Apply a warm compress to the area to soothe the skin. To prevent it in the future, use a fresh razor every time, use plenty of shaving cream, and shave in the direction of hair growth. Alternatively, consider trimming instead of shaving to avoid skin irritation entirely.
9. Latex Condoms or Lubricants
Sometimes the source of the itch is introduced during intimacy. Many women have a sensitivity or allergy to latex. If you notice itching or swelling immediately after or the day following sex with a condom, this could be the culprit. Similarly, some lubricants contain glycerin or parabens that can irritate sensitive tissues.
How to handle it: Try switching to non-latex condoms (such as polyisoprene or polyurethane) and use natural, water-based, or silicone-based lubricants that are free from fragrances and cooling/warming agents.
10. General Hygiene Issues
It sounds simple, but sometimes the itch is a result of trapped moisture. Wearing tight synthetic underwear, wet bathing suits, or sweaty workout clothes for too long creates a warm, damp environment where bacteria and yeast thrive. Conversely, over-cleaning (douching) can also cause itching by stripping the vagina of its natural protective flora.
How to handle it: Stick to cotton underwear that allows the area to breathe. Change out of sweaty gym clothes immediately after working out. Most importantly, remember that the vagina is a self-cleaning organ—you do not need to wash inside it. Cleaning the external vulva with warm water and mild, unscented soap is all that is necessary.
When to See a Doctor
While an occasional itch is normal, persistent itching that disrupts your life or comes with other symptoms (foul odor, strange discharge, pain, or sores) requires professional attention. Avoid the temptation to self-diagnose with leftover creams in your medicine cabinet. A quick trip to the gynecologist can ensure you treat the right problem and get back to feeling comfortable in your own skin.
Empowering Wellness: A Comprehensive Guide to Common Women’s Health Issues
Women’s health is a vast and dynamic field that encompasses far more than just reproductive well-being. While gynecological health is a cornerstone of a woman’s life, unique biological, hormonal, and physiological factors influence how women experience a wide range of medical conditions. From cardiovascular disease to autoimmune disorders, women often face distinct symptoms and risk factors that require specialized attention and awareness.
Understanding these health issues is the first step toward empowerment. By recognizing the signs of common conditions and prioritizing preventive care, women can take proactive steps to maintain their quality of life. This comprehensive guide explores the most prevalent health issues affecting women today and offers insights into prevention and management.
1. Heart Disease: The Leading Health Threat
There is a common misconception that heart disease is primarily a man’s issue. However, heart disease remains the leading cause of death for women globally. The biology of a woman’s heart differs slightly from a man’s, and consequently, the warning signs of a heart attack can be more subtle.
Recognizing the Symptoms
While chest pain is a classic symptom, women are more likely to experience atypical symptoms that can be easily dismissed as fatigue or the flu. These include:
- Shortness of breath
- Nausea or vomiting
- Back or jaw pain
- Extreme fatigue
- Dizziness or lightheadedness
Prevention: Maintaining a heart-healthy lifestyle is crucial. This includes regular cardiovascular exercise, a balanced diet low in saturated fats and sodium, smoking cessation, and managing stress levels. Regular screenings for blood pressure and cholesterol are essential for early detection.
2. Breast and Gynecological Cancers
Cancer remains a significant concern for women, with breast, cervical, ovarian, and uterine cancers being among the most common affecting the female population.
Breast Cancer
Breast cancer is the most diagnosed cancer in women. Early detection significantly improves survival rates. Women are encouraged to perform monthly self-exams to check for lumps or changes in skin texture. Furthermore, routine mammograms—typically starting at age 40 or earlier depending on family history—are vital for catching abnormalities before they become symptomatic.
Cervical and Ovarian Cancer
Cervical cancer is highly preventable thanks to the HPV vaccine and regular Pap smears, which can detect precancerous changes in the cervix. Ovarian cancer, often called the “silent killer,” is harder to detect because symptoms like bloating, pelvic pain, and urinary frequency can mimic other less serious conditions. Persistent symptoms should always be evaluated by a healthcare professional.
3. Reproductive Health Issues
Beyond pregnancy and childbirth, women’s reproductive systems are susceptible to various conditions that can impact daily life and fertility.

Endometriosis and Fibroids
Endometriosis occurs when tissue similar to the lining of the uterus grows outside of it, causing severe pain and potential fertility issues. Similarly, uterine fibroids are noncancerous growths of the uterus that can cause heavy menstrual bleeding and pelvic pressure. Both conditions often go undiagnosed for years, with women suffering in silence. Seeking a specialist’s opinion is key if menstrual pain interferes with daily activities.
Polycystic Ovary Syndrome (PCOS)
PCOS is a hormonal disorder common among women of reproductive age. It can cause irregular periods, excess androgen levels, and cysts on the ovaries. Beyond fertility, PCOS is linked to insulin resistance, increasing the risk of type 2 diabetes and heart disease later in life.
4. Osteoporosis and Bone Health
Osteoporosis is a disease that weakens bones, making them fragile and more likely to break. Women are significantly more likely to develop osteoporosis than men, particularly after menopause.
The Estrogen Connection
Estrogen plays a vital role in protecting bone density. When estrogen levels drop during menopause, bone loss accelerates. This makes older women particularly susceptible to fractures of the hip, spine, and wrist.
Prevention: Building strong bones starts early in life, but it is never too late to improve bone health. Key preventive measures include:
- Adequate intake of Calcium and Vitamin D.
- Weight-bearing exercises (like walking, jogging, or weightlifting).
- Limiting alcohol consumption and avoiding smoking.
- Bone density scans (DEXA) for women over 65 or those at high risk.
5. Autoimmune Diseases
Interestingly, autoimmune diseases—where the body’s immune system attacks healthy cells—disproportionately affect women. Conditions such as Lupus, Rheumatoid Arthritis, Multiple Sclerosis, and Thyroid disorders (Hashimoto’s and Graves’ disease) are far more prevalent in the female population.
Symptoms of autoimmune disorders can be vague and intermittent, often leading to a long road to diagnosis. Unexplained fatigue, joint pain, skin rashes, and low-grade fevers are common indicators that warrant a comprehensive medical evaluation.
6. Mental Health and Hormonal Fluctuations
Women are statistically more likely than men to experience anxiety and depression. While social and environmental factors play a role, biological factors are also significant. Hormonal fluctuations during the menstrual cycle, pregnancy, the postpartum period, and menopause can trigger or exacerbate mental health conditions.
Postpartum Depression (PPD): This is more than just the “baby blues.” PPD is a serious condition requiring medical attention. Similarly, the hormonal shifts during perimenopause can lead to mood swings, irritability, and depression.
It is vital to destigmatize mental health care. Therapy, support groups, and medication are effective tools, and prioritizing mental well-being is just as important as physical health.
The Importance of Preventive Screenings
The most effective tool in combating these women’s health issues is proactive care. Regular check-ups allow doctors to track changes in your health over time. A standard woman’s wellness exam typically includes:
- Pelvic exam and Pap smear
- Clinical breast exam
- Blood pressure and cholesterol check
- Screening for diabetes and thyroid issues
- Discussions about mental health and lifestyle
Conclusion
Women’s health is complex, influenced by a blend of genetics, hormones, and lifestyle. While the risk of conditions like heart disease, cancer, and osteoporosis is real, knowledge is the ultimate defense. By listening to your body, maintaining a healthy lifestyle, and adhering to recommended screening schedules, you can navigate these challenges effectively.
If you are experiencing symptoms or are overdue for a check-up, do not wait. Prioritize your health today to ensure a vibrant and active tomorrow.

Uterine Prolapse Explained: Symptoms, Causes, and Effective Treatments
For many women, pelvic health is a topic often shrouded in silence, yet conditions affecting the pelvic floor are incredibly common. One such condition, uterine prolapse, affects millions of women worldwide, impacting their daily comfort, activity levels, and overall quality of life. While the sensation of pelvic pressure or tissue protrusion can be alarming, it is a treatable condition. Understanding the anatomy, causes, and available solutions is the first step toward reclaiming your confidence and comfort.

Uterine prolapse occurs when the pelvic floor muscles and ligaments stretch and weaken, providing inadequate support for the uterus. The uterus then slips down into or protrudes out of the vagina. To visualize this, think of your pelvic floor muscles as a hammock that holds your pelvic organs—the uterus, bladder, and bowel—in place. When this hammock loses its elasticity or strength, it can no longer suspend these organs effectively.
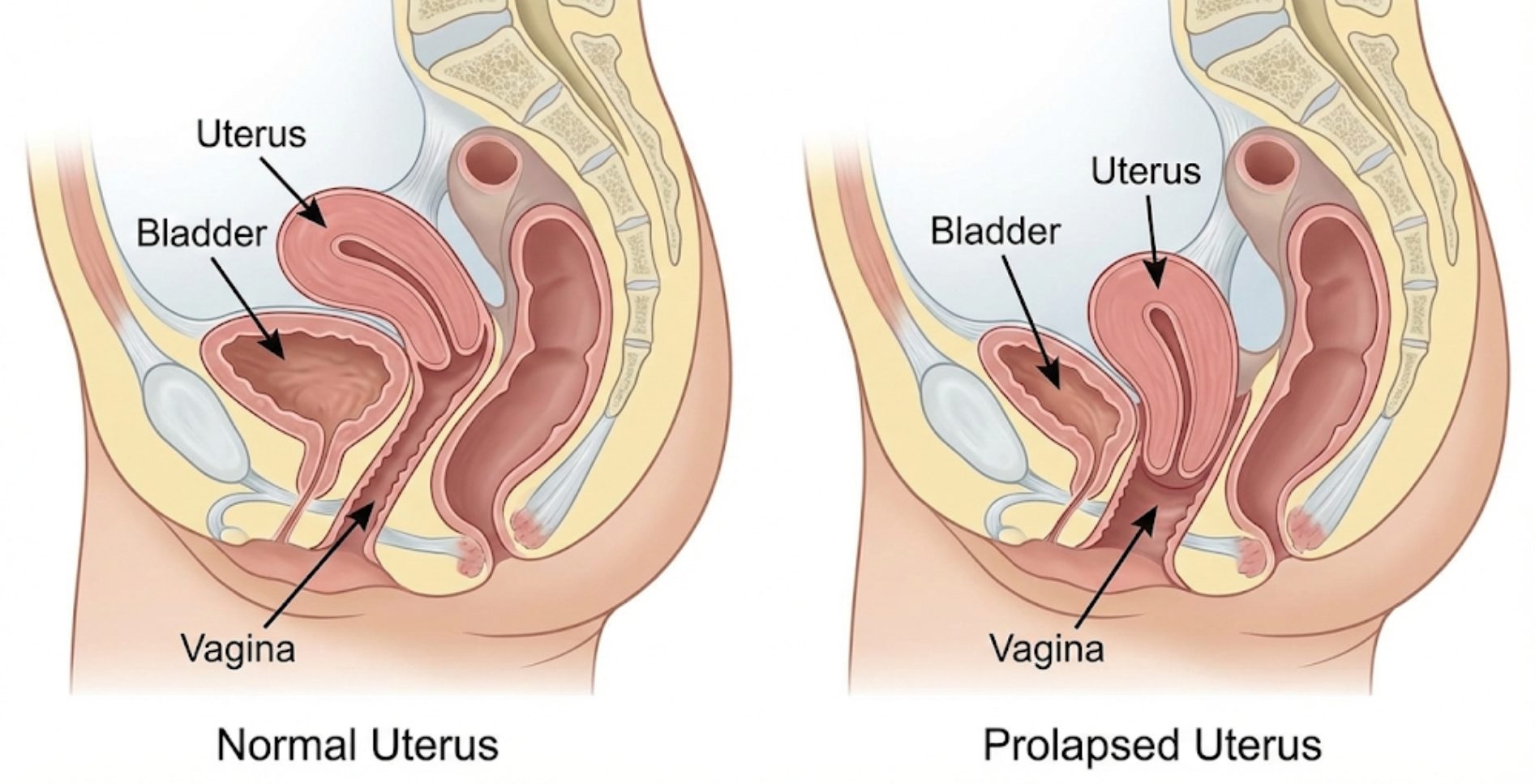
This condition can affect women of any age, though it is significantly more prevalent in postmenopausal women who have had one or more vaginal deliveries. The severity of the prolapse can range from mild (where the uterus drops slightly) to severe (where the uterus protrudes significantly outside the vaginal opening).
In mild cases, uterine prolapse may not present any noticeable symptoms. However, as the condition progresses, the physical sensations can become hard to ignore. Symptoms often worsen as the day goes on or after long periods of standing.
Common signs and symptoms include:
Because the pelvic organs are closely packed together, the displacement of the uterus often affects the bladder and bowel. You might experience:
Uterine prolapse is fundamentally caused by the weakening of pelvic muscles and supportive tissues. Several factors contribute to this structural failure.
The most significant risk factor is pregnancy and childbirth. The weight of the baby during pregnancy and the strain of vaginal delivery can stretch and damage the pelvic floor nerves and tissues. Women who have had multiple vaginal births, large babies, or difficult labors are at higher risk.
As women age, the production of estrogen decreases naturally, particularly during and after menopause. Estrogen plays a vital role in maintaining the strength and elasticity of collagen, the connective tissue that supports the pelvic organs. Lower estrogen levels lead to weaker pelvic tissues.
Any activity or condition that puts repeated pressure on the abdomen can strain the pelvic floor over time. This includes:
Diagnosing uterine prolapse is typically straightforward and involves a pelvic examination. During the exam, your doctor will likely ask you to bear down as if having a bowel movement to see how far the uterus has descended. They may also ask you to tighten your pelvic muscles to assess their strength. In some cases, questionnaires regarding urinary function and quality of life help the doctor understand the impact of the condition on your daily routine.
The treatment for uterine prolapse depends on the severity of the condition and how much it bothers you. If you have a mild prolapse with no symptoms, medical treatment might not be necessary immediately, but lifestyle changes are recommended to prevent worsening.
For mild to moderate cases, or for women who wish to avoid surgery, several effective options exist:
If the prolapse is severe or non-surgical methods fail to provide relief, surgery may be recommended. Options include:
While you cannot control genetic factors or the natural aging process, you can take steps to protect your pelvic floor:
Uterine prolapse is not a condition you have to live with in silence. It is a mechanical issue with effective medical solutions. If you are experiencing symptoms like pelvic pressure, tissue protrusion, or urinary difficulties, consult your healthcare provider. With the right combination of lifestyle changes, therapies, or medical interventions, you can restore your comfort and return to an active, worry-free life.
What is Uterine Prolapse?
Recognizing the Symptoms
- Sensation of Heaviness: Many women describe a feeling of heaviness or pulling in the pelvis.
- Tissue Protrusion: Seeing or feeling tissue bulging out of the vagina is a hallmark symptom of more advanced prolapse.
- The “Ball” Sensation: A distinct feeling as if you are sitting on a small ball.
- Sexual Discomfort: Sensations of looseness in the vaginal tissue or pain during intercourse.
- Lower Back Pain: A dull ache in the lower back that may subside when lying down.
Urinary and Bowel Complications
- Urinary Incontinence: Leakage of urine when coughing, sneezing, or laughing (stress incontinence).
- Retention: Difficulty emptying the bladder completely, which can increase the risk of urinary tract infections.
- Bowel Movement Issues: Constipation or difficulty passing a bowel movement without applying pressure to the vagina (splinting).
The Primary Causes and Risk Factors
Pregnancy and Childbirth
Aging and Menopause
Chronic Intra-abdominal Pressure
- Obesity: Excess weight puts continuous strain on pelvic muscles.
- Chronic Coughing: Conditions like bronchitis or smoker’s cough create repeated downward pressure.
- Chronic Constipation: Straining during bowel movements is a major contributor to prolapse.
- Heavy Lifting: Jobs or exercises that involve repeated heavy lifting can accelerate muscle weakening.
Diagnosis
Treatment Options: From Self-Care to Surgery
Non-Surgical Approaches
- Kegel Exercises: These are targeted exercises designed to strengthen the pelvic floor muscles. By regularly tightening and relaxing these muscles, you can reinforce the “hammock” supporting the uterus. While Kegels may not reverse severe prolapse, they can prevent mild cases from worsening and alleviate symptoms.
- Vaginal Pessary: A pessary is a plastic or rubber ring inserted into the vagina to support the bulging tissues. It works somewhat like a structural prop. Pessaries come in various shapes and sizes and must be fitted by a healthcare provider. They can be a permanent solution or a temporary measure while deferring surgery.
- Estrogen Therapy: For postmenopausal women, using vaginal estrogen (cream, ring, or tablet) can help restore some vitality and strength to the vaginal tissues, although it does not fix the structural prolapse itself.
Surgical Interventions
- Tissue Repair: This involves grafting your own tissue, donor tissue, or synthetic material onto weakened pelvic floor structures to support the pelvic organs. This is often done through the vagina but can be laparoscopic.
- Hysterectomy: In severe cases, the uterus itself may be removed. While this corrects the uterine prolapse, surgeons must also address the vaginal vault to prevent it from prolapsing in the future.
Prevention and Lifestyle Management
- Maintain a Healthy Weight: Reducing excess body weight reduces the load on your pelvic floor.
- Treat Constipation: Eat a high-fiber diet and drink plenty of fluids to ensure soft stools and avoid straining.
- Practice Proper Lifting: Avoid lifting heavy objects, and when you must, lift with your legs, not your waist or back.
- Quit Smoking: Eliminating the chronic “smoker’s cough” can significantly reduce pelvic pressure.
Conclusion

Overcoming the Breastfeeding Challenge: Solutions for Common Struggles
Breastfeeding is often described as one of the most natural things in the world. While this is true, describing it as "natural" can sometimes obscure the fact that it is also a learned skill—both for the mother and the baby. For many new parents, the journey is filled with tender moments of connection, but it can also present a significant breastfeeding challenge that tests their patience and resilience.
According to global health organizations, breast milk provides the optimal nutrition for infants. However, the pressure to breastfeed exclusively can be overwhelming when things don’t go according to plan. Whether you are in the first few days postpartum or navigating a sleep regression months down the line, encountering obstacles is normal. The good news is that most of these hurdles are temporary and solvable with the right knowledge and support.
Drawing on expert guidance, including insights from UNICEF, we have compiled a comprehensive guide to navigating the five most common breastfeeding problems. If you are feeling discouraged, take a deep breath; you are not alone, and there are solutions available.
1. The Challenge of Sore and Cracked Nipples
One of the most immediate hurdles new mothers face is nipple pain. While some tenderness is common in the first few days as your nipples adjust, breastfeeding should not be excruciatingly painful. If you are curling your toes every time your baby latches, it is usually a sign that something needs adjustment.
The Root Cause: Attachment
In the vast majority of cases, sore or cracked nipples are caused by a poor latch (attachment). If the baby is sucking on the nipple alone rather than taking a large mouthful of breast tissue, it causes friction and damage.
How to Fix It
- Check the Position: Ensure your baby’s mouth is wide open before they latch. Their chin should be touching your breast, and their nose should be clear. You want the nipple to go deep into the roof of their mouth.
- Break the Suction: If it hurts, do not just pull the baby off. Gently insert your clean pinky finger into the corner of the baby’s mouth to break the suction before trying again.
- Aftercare: After feeding, you can rub a little breast milk on your nipples and let them air dry. Breast milk has natural healing properties. Avoid using harsh soaps or scrubbing the area, as this can dry out the skin further.
2. Worries About Low Milk Supply
Perhaps the most anxiety-inducing breastfeeding challenge is the fear that you are not producing enough milk. This is one of the top reasons mothers stop breastfeeding earlier than they intended. However, perception often differs from reality.
Understanding Supply and Demand
Breast milk production works on a supply and demand basis. The more the baby feeds, the more milk your body makes. In the early days, it is normal for a baby to feed very frequently (cluster feeding). This does not necessarily mean they are starving; they are signaling your body to ramp up production.
Signs Your Baby is Getting Enough
Instead of focusing on how full your breasts feel, look at the baby:
- Diaper Output: A well-fed baby will have plenty of wet and dirty diapers (usually at least 6 heavy wet diapers a day after the first week).
- Weight Gain: Your pediatrician will track the baby’s growth curve. Consistent weight gain is the best indicator of supply.
- Alertness: Is the baby active and alert when awake?
If you are truly concerned about supply, continue to feed on demand and consult a lactation consultant before supplementing with formula, as supplementation can interrupt the supply-demand loop.
3. Dealing with Engorgement
When your milk "comes in" (usually days 2-5 postpartum), your breasts may become hard, swollen, and uncomfortable. This is known as engorgement. It can make it difficult for the baby to latch because the breast tissue is so taut.
Relief Strategies
To manage this breastfeeding challenge, the goal is to keep the milk flowing without overstimulating production excessively.
- Feed Frequently: Do not skip feedings. Emptying the breast is the primary way to relieve pressure.
- Hand Expression: If the breast is too hard for the baby to latch, gently hand express a small amount of milk to soften the areola before offering the breast.
- Cold Compresses: Applying a cold compress or chilled cabbage leaves (a traditional remedy supported by some anecdotal evidence) between feeds can help reduce swelling and inflammation.
4. Blocked Milk Ducts
A blocked duct feels like a small, tender lump in the breast. It occurs when milk is not draining completely from a specific area. If left untreated, a blocked duct can lead to mastitis, so it is important to address it immediately.
Clearing the Blockage
- Heat and Massage: Apply a warm compress to the affected area before feeding. While the baby is nursing, gently massage the lump toward the nipple to help move the milk.
- Positioning: Try changing breastfeeding positions. Pointing the baby’s chin toward the lump can help drain that specific area of the breast more effectively.
- Loose Clothing: Ensure your bra is not too tight, as external pressure can contribute to blocked ducts.
5. Mastitis: When to See a Doctor
If a blocked duct is not cleared, or if bacteria enters the breast tissue through a cracked nipple, it can lead to mastitis—an inflammation of the breast that may involve an infection.
Recognizing the Symptoms
Mastitis often feels like the flu. Symptoms include:
- A red, hot, and painful area on the breast.
- Fever and chills.
- General fatigue and body aches.
Treatment
If you suspect mastitis, it is crucial to see a healthcare provider. While you may need antibiotics, it is generally safe and recommended to continue breastfeeding from the affected side to keep the milk flowing. Sudden weaning during mastitis can make the infection worse by causing milk stasis. Rest and hydration are also vital for recovery.
Emotional Resilience and Support
Beyond the physical mechanics, the mental aspect of the breastfeeding challenge is significant. Sleep deprivation combined with hormonal shifts can make even small problems feel insurmountable.
It is essential to build a support village. This might include a partner who handles diaper changes and burping, a friend who brings meals, or a professional lactation consultant who can offer hands-on help. Remember, asking for help is not a sign of weakness; it is a strategy for success.
Conclusion
Every mother’s journey is unique. Whether you breastfeed for two days, two months, or two years, your effort matters. By understanding these common issues—sore nipples, low supply concerns, engorgement, blocked ducts, and mastitis—you are better equipped to handle them if they arise.
If you are currently in the thick of a breastfeeding challenge, take it one feed at a time. Trust your body, watch your baby, and reach out to healthcare professionals like those at UNICEF or local lactation experts whenever you need guidance. You are doing a remarkable job.

The Best Positions for Breastfeeding: A Comprehensive Guide for Comfort and Latch
Breastfeeding is often described as one of the most natural things in the world. However, for many new mothers, it can feel anything but natural in the beginning. It is a learned skill that takes practice, patience, and a bit of experimentation for both you and your baby. One of the most critical factors in establishing a successful breastfeeding journey is finding the best position for breastfeeding that works for your unique anatomy and your baby’s needs.
While there is no single "perfect" way to nurse, understanding the variety of positions available can make a world of difference in preventing sore nipples, ensuring a deep latch, and making feeding time a relaxing bonding experience. Whether you are recovering from a C-section, nursing twins, or simply trying to get comfortable, this guide explores the most effective breastfeeding positions recommended by experts.
Why Positioning Matters
Before diving into the specific holds, it is important to understand why positioning is so crucial. A good position supports effective latching, which is the key to transferring milk efficiently and preventing pain. If a mother is uncomfortable, her muscles tense up, which can inhibit the let-down reflex. Similarly, if a baby feels unstable, they may clamp down on the nipple or struggle to swallow.
Regardless of the position you choose, keep these universal tips in mind:
- Bring the baby to the breast, not the breast to the baby. Hunching over can cause back pain and shallow latches.
- Alignment is key. The baby’s head, shoulders, and hips should be in a straight line. They should not have to turn their head to reach the nipple.
- Nose to nipple. Start with the baby’s nose opposite your nipple to encourage them to tilt their head back and open their mouth wide.
1. Laid-Back Breastfeeding (Biological Nurturing)
Often considered the best starting point for newborns, laid-back breastfeeding taps into the baby’s natural instincts. This position allows gravity to help keep the baby in place, rather than you having to support their weight entirely with your arms.
How to do it:
Find a comfortable bed or couch and lean back in a semi-reclined position. Make sure your back and head are well-supported with pillows. Place your baby tummy-to-tummy on your chest. Gravity keeps the baby secure, allowing them to use their innate reflexes to scoot up, root, and latch onto the breast.
Why try this? It is excellent for the early days when you are tired or recovering from birth. It also helps babies who struggle to latch in more upright positions.
2. The Cradle Hold
This is the classic position most people imagine when they think of breastfeeding. While it is popular, it requires good head control from the baby or careful support from the mother, so it may be easier once the baby is a few weeks old.
How to do it:
Sit upright in a comfortable chair with armrests. Hold your baby across your lap, tummy-to-tummy. The baby’s head should rest in the crook of your elbow on the side you are nursing from. Use your forearm to support their back and your hand to support their bottom.
Pro Tip: Use a nursing pillow or cushion to raise the baby to nipple height so you don’t have to lean forward or lift your arm too high, which can cause shoulder strain.
3. The Cross-Cradle Hold
The cross-cradle hold is very similar to the cradle hold but offers more control over the baby’s head. This makes it one of the best positions for breastfeeding newborns or babies who have difficulty latching.
How to do it:
Sit upright. If you are nursing on the left breast, use your right arm to hold the baby. Support the baby’s body with your forearm and hold the base of their head (below the ears) with your hand. Use your left hand to shape your breast. This gives you maximum visibility and control to guide the baby’s mouth to the nipple.
4. The Underarm (Rugby Ball or Clutch) Hold
As the name suggests, you hold the baby under your arm like a rugby ball or a handbag. This position is a favorite for mothers who have had a Caesarean section because it keeps the baby away from the incision site.
How to do it:
Sit with a pillow at your side. Tuck the baby under your arm on the side you are nursing from. Their hips should be near your hip, and their legs should extend behind you. Support the baby’s neck and shoulders with your hand and their upper back with your forearm. Guide them to the nipple, ensuring their nose is level with it.
Why try this? Aside from C-section recovery, this hold is fantastic for women with larger breasts or for nursing twins in tandem.
5. Side-Lying Position
For night feeds or mothers who need extra rest, the side-lying position is a lifesaver. It allows you to nurse while lying down, maximizing rest for both you and the baby.
How to do it:
Lie on your side on a bed, facing your baby. Your baby should also be on their side, facing you, tummy-to-tummy. You can place a pillow behind your back for support and perhaps a small rolled-up towel behind the baby to keep them from rolling away. Align the baby’s mouth with your nipple. You may need to lift your breast slightly with your hand to help them latch initially.
Safety Note: Ensure the sleeping surface is firm and flat, and remove excess bedding around the baby to follow safe sleep guidelines.
6. The Koala Hold (Upright Breastfeeding)
In this position, the baby straddles your thigh or sits on your hip while feeding. It is an older baby favorite but can be done with newborns if plenty of support is provided.
How to do it:
Sit the baby on your thigh, facing you. Support their back and head with one hand while offering the breast with the other. This is essentially a vertical version of the cradle hold.
Why try this? This is often the best position for babies suffering from reflux or ear infections, as the upright angle helps keep milk down and reduces pressure in the ears.
Troubleshooting Your Position
Even with the right position, challenges can arise. If you experience pain, unlatch the baby gently by inserting a clean finger into the corner of their mouth to break the suction and try again. Look for signs of effective feeding, such as rhythmic sucking, swallowing sounds, and the baby appearing satisfied after the feed.
Remember, the "best" position is simply the one that works for you and your baby at that moment. As your baby grows and gains head control, your preferred positions will likely change. Don’t hesitate to use pillows, footstools, and armrests to build a comfortable nest for yourself.
If you continue to struggle with positioning or latching, consult a lactation consultant or a healthcare provider. Organizations like UNICEF provide excellent resources and visual guides to help parents navigate these early challenges. Breastfeeding is a journey, and finding your groove takes time—be patient with yourself and your little one.

