Understanding Uterine Prolapse: Symptoms, Causes, and Effective Treatments
Uterine prolapse is a medical condition that affects many women, yet it remains a topic often shrouded in silence due to embarrassment or lack of awareness. Simply put, uterine prolapse (known as 子宫下垂 in Chinese medical contexts) occurs when the pelvic floor muscles and ligaments stretch and weaken, providing inadequate support for the uterus. Consequently, the uterus slips down into or protrudes out of the vagina.
While this condition can affect women of any age, it is most common in postmenopausal women who have had one or more vaginal deliveries. Understanding the signs, causes, and treatment options is crucial for maintaining long-term pelvic health and quality of life.
What Exactly is Uterine Prolapse?
The uterus (womb) is normally held in place inside the pelvis with various muscles, tissue, and ligaments. Think of these support structures as a hammock. When this hammock weakens or gets damaged, it can no longer hold the uterus in its proper position. Gravity takes over, and the uterus descends toward the vaginal opening.
Prolapse can range from mild to severe:
- First degree: The cervix drops into the vagina.
- Second degree: The cervix drops to the level just inside the opening of the vagina.
- Third degree: The cervix is outside the vagina.
- Fourth degree: The entire uterus is outside the vagina (procidentia).
Identifying the Symptoms
In mild cases, women may not experience any noticeable symptoms. However, as the condition progresses, the signs become more apparent and can significantly impact daily life. Common symptoms include:
- A sensation of heaviness or pulling in the pelvis.
- Tissue protruding from the vagina, often described as feeling like you are sitting on a small ball.
- Urinary problems, such as urine leakage (incontinence) or urine retention (inability to empty the bladder completely).
- Trouble having a bowel movement.
- Lower back pain that often worsens as the day goes on.
- Sexual concerns, such as a sensation of looseness in the tone of your vaginal tissue.
Symptoms are often less bothersome in the morning and worsen as the day progresses due to the effects of gravity.
Causes and Risk Factors
Several factors contribute to the weakening of the pelvic floor muscles, leading to uterine prolapse. It is rarely caused by a single event but rather a combination of factors over time.
1. Pregnancy and Childbirth
This is the most significant risk factor. Pregnancy puts immense strain on the pelvic floor, and vaginal childbirth—especially with a large baby or difficult labor—can stretch and tear the supportive tissues. The damage may not manifest as prolapse until years later.
2. Aging and Menopause
As women age, the natural production of estrogen decreases. Estrogen helps keep the pelvic muscles strong and elastic. During menopause, the drop in estrogen levels leads to thinner, less resilient pelvic tissues, increasing the risk of prolapse.
3. Chronic Strain
Any activity that puts repeated pressure on the abdomen can weaken pelvic muscles. This includes:
- Chronic coughing (often associated with smoking or lung conditions).
- Straining during bowel movements (chronic constipation).
- Heavy lifting, whether for exercise, work, or daily chores.
4. Obesity
Excess body weight places additional strain on the pelvic floor muscles, accelerating their weakening.
Diagnosis and Treatment Options
If you suspect you have uterine prolapse, consulting a healthcare provider is essential. Diagnosis is usually confirmed through a pelvic examination. Treatment depends on the severity of the prolapse and how much the symptoms affect your life.
Non-Surgical Treatments
For mild to moderate cases, or for women who wish to avoid surgery, conservative treatments are often effective:
- Lifestyle Changes: Losing weight, treating constipation, and avoiding heavy lifting can reduce pressure on the pelvic floor.
- Kegel Exercises: These exercises strengthen the pelvic floor muscles. When performed correctly and consistently, they can halt the progression of prolapse and alleviate symptoms.
- Vaginal Pessary: A plastic or rubber ring inserted into the vagina to support the bulging tissues. This is a common non-surgical solution that requires regular cleaning.
Surgical Interventions
For severe cases where conservative measures fail, surgery may be recommended. Options generally include:
- Tissue Repair: Grafting your own tissue, donor tissue, or synthetic material onto the weakened pelvic floor structures to support the pelvic organs.
- Hysterectomy: The removal of the uterus. This is often considered when the prolapse is severe and the woman does not plan to have more children.
Prevention and Outlook
While you cannot control genetic factors or aging, you can take steps to protect your pelvic floor. Maintaining a healthy weight, treating chronic coughs promptly, avoiding constipation through a high-fiber diet, and regularly performing pelvic floor exercises are the best defenses against uterine prolapse.
Uterine prolapse is a treatable condition. With the right medical guidance and lifestyle adjustments, women can regain their comfort and confidence. If you are experiencing symptoms, do not suffer in silence—reach out to a gynecologist to discuss the best path forward for your health.

Uterine Prolapse Explained: Symptoms, Causes, and Effective Treatments
For many women, pelvic health is a topic often shrouded in silence, yet conditions affecting the pelvic floor are incredibly common. One such condition, uterine prolapse, affects millions of women worldwide, impacting their daily comfort, activity levels, and overall quality of life. While the sensation of pelvic pressure or tissue protrusion can be alarming, it is a treatable condition. Understanding the anatomy, causes, and available solutions is the first step toward reclaiming your confidence and comfort.

Uterine prolapse occurs when the pelvic floor muscles and ligaments stretch and weaken, providing inadequate support for the uterus. The uterus then slips down into or protrudes out of the vagina. To visualize this, think of your pelvic floor muscles as a hammock that holds your pelvic organs—the uterus, bladder, and bowel—in place. When this hammock loses its elasticity or strength, it can no longer suspend these organs effectively.
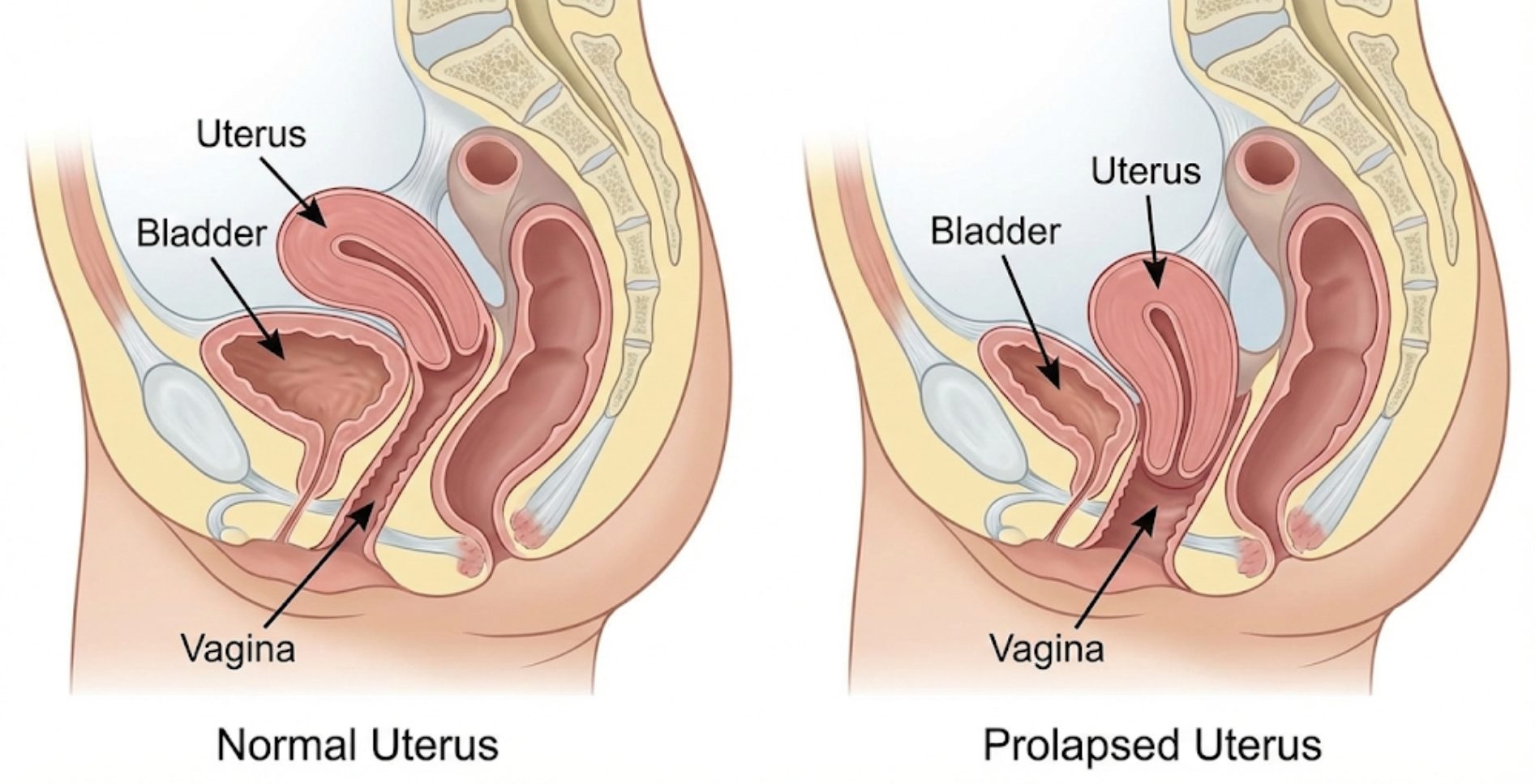
This condition can affect women of any age, though it is significantly more prevalent in postmenopausal women who have had one or more vaginal deliveries. The severity of the prolapse can range from mild (where the uterus drops slightly) to severe (where the uterus protrudes significantly outside the vaginal opening).
In mild cases, uterine prolapse may not present any noticeable symptoms. However, as the condition progresses, the physical sensations can become hard to ignore. Symptoms often worsen as the day goes on or after long periods of standing.
Common signs and symptoms include:
Because the pelvic organs are closely packed together, the displacement of the uterus often affects the bladder and bowel. You might experience:
Uterine prolapse is fundamentally caused by the weakening of pelvic muscles and supportive tissues. Several factors contribute to this structural failure.
The most significant risk factor is pregnancy and childbirth. The weight of the baby during pregnancy and the strain of vaginal delivery can stretch and damage the pelvic floor nerves and tissues. Women who have had multiple vaginal births, large babies, or difficult labors are at higher risk.
As women age, the production of estrogen decreases naturally, particularly during and after menopause. Estrogen plays a vital role in maintaining the strength and elasticity of collagen, the connective tissue that supports the pelvic organs. Lower estrogen levels lead to weaker pelvic tissues.
Any activity or condition that puts repeated pressure on the abdomen can strain the pelvic floor over time. This includes:
Diagnosing uterine prolapse is typically straightforward and involves a pelvic examination. During the exam, your doctor will likely ask you to bear down as if having a bowel movement to see how far the uterus has descended. They may also ask you to tighten your pelvic muscles to assess their strength. In some cases, questionnaires regarding urinary function and quality of life help the doctor understand the impact of the condition on your daily routine.
The treatment for uterine prolapse depends on the severity of the condition and how much it bothers you. If you have a mild prolapse with no symptoms, medical treatment might not be necessary immediately, but lifestyle changes are recommended to prevent worsening.
For mild to moderate cases, or for women who wish to avoid surgery, several effective options exist:
If the prolapse is severe or non-surgical methods fail to provide relief, surgery may be recommended. Options include:
While you cannot control genetic factors or the natural aging process, you can take steps to protect your pelvic floor:
Uterine prolapse is not a condition you have to live with in silence. It is a mechanical issue with effective medical solutions. If you are experiencing symptoms like pelvic pressure, tissue protrusion, or urinary difficulties, consult your healthcare provider. With the right combination of lifestyle changes, therapies, or medical interventions, you can restore your comfort and return to an active, worry-free life.
What is Uterine Prolapse?
Recognizing the Symptoms
- Sensation of Heaviness: Many women describe a feeling of heaviness or pulling in the pelvis.
- Tissue Protrusion: Seeing or feeling tissue bulging out of the vagina is a hallmark symptom of more advanced prolapse.
- The “Ball” Sensation: A distinct feeling as if you are sitting on a small ball.
- Sexual Discomfort: Sensations of looseness in the vaginal tissue or pain during intercourse.
- Lower Back Pain: A dull ache in the lower back that may subside when lying down.
Urinary and Bowel Complications
- Urinary Incontinence: Leakage of urine when coughing, sneezing, or laughing (stress incontinence).
- Retention: Difficulty emptying the bladder completely, which can increase the risk of urinary tract infections.
- Bowel Movement Issues: Constipation or difficulty passing a bowel movement without applying pressure to the vagina (splinting).
The Primary Causes and Risk Factors
Pregnancy and Childbirth
Aging and Menopause
Chronic Intra-abdominal Pressure
- Obesity: Excess weight puts continuous strain on pelvic muscles.
- Chronic Coughing: Conditions like bronchitis or smoker’s cough create repeated downward pressure.
- Chronic Constipation: Straining during bowel movements is a major contributor to prolapse.
- Heavy Lifting: Jobs or exercises that involve repeated heavy lifting can accelerate muscle weakening.
Diagnosis
Treatment Options: From Self-Care to Surgery
Non-Surgical Approaches
- Kegel Exercises: These are targeted exercises designed to strengthen the pelvic floor muscles. By regularly tightening and relaxing these muscles, you can reinforce the “hammock” supporting the uterus. While Kegels may not reverse severe prolapse, they can prevent mild cases from worsening and alleviate symptoms.
- Vaginal Pessary: A pessary is a plastic or rubber ring inserted into the vagina to support the bulging tissues. It works somewhat like a structural prop. Pessaries come in various shapes and sizes and must be fitted by a healthcare provider. They can be a permanent solution or a temporary measure while deferring surgery.
- Estrogen Therapy: For postmenopausal women, using vaginal estrogen (cream, ring, or tablet) can help restore some vitality and strength to the vaginal tissues, although it does not fix the structural prolapse itself.
Surgical Interventions
- Tissue Repair: This involves grafting your own tissue, donor tissue, or synthetic material onto weakened pelvic floor structures to support the pelvic organs. This is often done through the vagina but can be laparoscopic.
- Hysterectomy: In severe cases, the uterus itself may be removed. While this corrects the uterine prolapse, surgeons must also address the vaginal vault to prevent it from prolapsing in the future.
Prevention and Lifestyle Management
- Maintain a Healthy Weight: Reducing excess body weight reduces the load on your pelvic floor.
- Treat Constipation: Eat a high-fiber diet and drink plenty of fluids to ensure soft stools and avoid straining.
- Practice Proper Lifting: Avoid lifting heavy objects, and when you must, lift with your legs, not your waist or back.
- Quit Smoking: Eliminating the chronic “smoker’s cough” can significantly reduce pelvic pressure.

